Compliance Monitoring for Scoliosis Brace Treatment
Compliance Monitoring for Scoliosis Brace Treatment
By Jennifer Johansson, MS
The goal of brace treatment for adolescent idiopathic scoliosis (AIS) is to stop the progression of the curve as bracing does not typically reduce the degree of the curve already present. AIS braces are prescribed to be worn tightly and for many hours per day. A patient that is still growing with a curve of 25-30 degrees can be prescribed a brace for up to 23 hours per day until he or she has stopped growing (skeletal maturity), typically anywhere from two to 42 months.1
It has just been in this decade that ground-breaking studies have confirmed the efficacy of this treatment.1,2 Katz et al.’s landmark study1 found that 82 percent of patients who wore their brace more than 12 hours per day had a favorable outcome (curve progression <6 degrees) as compared to only 31 percent of those who wore their brace less than seven hours per day (p=0.0005). The Bracing in Adolescent Idiopathic Scoliosis Trial (BrAIST), a multicenter, randomized clinical trial funded by the National Institutes of Health (NIH), was stopped early owing to the efficacy of bracing and confirmed Katz’s results with a treatment success (curve progression <6 degrees) rate of 90-93 percent with at least 12.9 hours of daily brace wear.2 The studies not only indicated that brace treatment was more effective than observation, but that longer hours of wear were associated with greater benefit. In light of this evidence, ensuring the proper wear of a scoliosis brace is even more crucial than ever.
However, wear time is not the only factor in a successful treatment. The brace also must be worn at the prescribed tightness of fit. Without both of these criteria being met, the effectiveness of the brace treatment is compromised. For example, one patient could wear the brace 23 hours per day but never achieve the correct fit, so the corrective forces are minimal or nonexistent. Conversely, another patient could wear the brace as tight as prescribed but only for one hour per day. In neither case is the patient going to achieve optimal outcomes from the brace treatment.
Given the prescription for long hours of wear of a tightly fitting brace, it is no surprise that user compliance can be an issue. The traditional means of assessing compliance are largely subjective and unreliable, utilizing questionnaires, verbal reporting to a clinician by the patient or parent, and/or assessing the braces for signs of wear. More quantitative thermal monitoring devices, such as the Cricket, Orthotimer, and iButton, are commercially available; however, these have seen limited use. One contributing factor for this may be that these devices only yield limited compliance data, measuring only wear time, and have no measure of how effectively the orthosis is donned during each period of wear (i.e., the tightness of fit). While few wear time monitors exist, even fewer systems are available that can measure both aspects of compliance. The Cinch Smart Strap has recently come on the market but also has seen limited buy-in from the community.
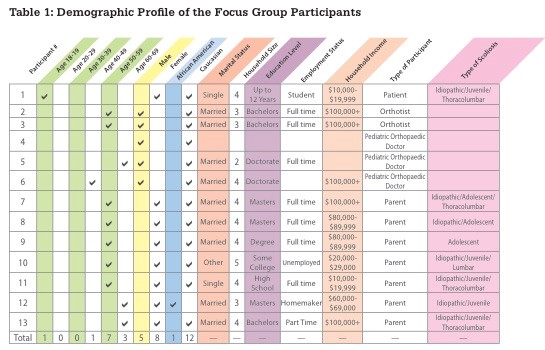
Therefore, to explore why these systems are not being fully embraced and better understand the need for such a system and how to meet that need, we enlisted the aid of the Center for Knowledge Translation for Technology Transfer (KT4TT) to perform a focus group. The experienced team ran a focus group of 13 participants comprised of clinicians, orthotists, parents of AIS patients, and former patients. The demographic profile of the participants is shown in Table 1.
Initially, the focus group confirmed many of our initial assumptions on the current challenges of brace treatment. The group noted that brace treatment often is not fully utilized for a variety of reasons and that kids can be very resourceful in not wearing the brace. They will take the brace off to eat, because they are hot, or even during the night while sleeping, often unconsciously, because it is uncomfortable. The group confirmed that compliance is a key issue, whether it be that the braces are often not worn securely enough or that they aren’t being worn long enough, and traditional means of measuring compliance like self-reporting on the part of the patient and/or parents are not accurate.
When asked what features they would look for in a compliance monitoring system, to assist both the user and the treating clinician to ensure optimal wear and maximize results, the group identified 13 key features (Table 2). Many of the features identified were as expected, such as being able to monitor both wear time (1) and tightness of fit (2), having a mobile app (5) to alert both the patient and parent or caregiver of incorrect fit (6), being inconspicuous (9) and robust (13), and being able to charge quickly (10) and provide battery status (11).
However, some of the reported features were less obvious. For example, it was important to the parents in the group that they could measure the body temperature of the patient (3) as overheating while wearing the brace was a concern. It also was important for the system to identify why the brace was not being worn correctly and provide a visual representation (7) to guide how to correct the fit—e.g., identify the strap(s) to tighten. Another desired feature was for the system to be able to measure improvements in the curvature of the spine when the brace was being worn (4). Currently this is done with in-brace X-rays so this may not be as easy to achieve as some of the other features. However, it is likely more straightforward to design a system that can be worn during X-rays (12). The final feature the group desired was that the system provide positive feedback to the brace wearer through the phone app. This was seen as a very important way to help motivate kids to wear the brace. By creating goals and rewards, such as app credits for an app store, gift cards, etc., when goals are reached, the hope is to engage the kids in the process.
While some of these features are easier to implement than others, 100 percent of the focus group stated that they would recommend use of, or want to use, a compliance monitoring system that met all of these key features. They believed such a system could reduce arguing over brace wear, take the parents/caregivers out of the role of bad guy, and achieve buy-in from the patients themselves to ultimately achieve the best possible outcomes from their brace treatment.
Unfortunately, one of the big hurdles for any new technology in this industry is reimbursement, and a compliance monitoring system is no different. Multiple times during the focus group, the participants indicated that affordability is key. When the focus group was asked how much this ideal system—with all of the key features—should cost, the responses ranged from $0 to $1,000, with a mean price of $296 and median price of $100. This speaks to the importance of cost—that more than half of the participants could not, or would not, pay more than $100 out-of-pocket for a system that could help ensure the best possible outcomes of a treatment designed to avoid spinal surgery for children.
Currently no insurance code exists that would cover the cost of such a system. Certainly, applying for a new L code would be a means of obtaining insurance reimbursement if the L code is approved; however, it is an arduous process that is not guaranteed to be successful. One suggestion from the group to help motivate insurers to cover the cost of the system was that brace wear should be tied to reimbursement; the more you wear it, the less you have to pay for the brace. Another was that if the system could determine if improper fit was due to the child outgrowing the brace, the compliance monitoring system could provide quantitative justification to insurance for the coverage of a new brace.
In conclusion, while the focus group agreed on the need for a compliance monitoring system and identified a variety of features an ideal system should have, some of the features are technically challenging, and there were definite discrepancies on what a reasonable out-of-pocket cost for such a system should be. However, despite these challenges, the research and development team at Liberating Technologies is working to develop an affordable solution based on the feedback from the focus group. Our solution, presented in more detail at the 2018 AOPA National Assembly in Vancouver, is an easily integrable, battery-powered system that consists of low-profile sensors to monitor forces in multiple locations, custom algorithms to determine wear time and tightness of fit, and a mobile app to provide feedback. Regardless of the technical challenges and reimbursement hurdles in developing this system, we believe it worthwhile in order to reduce the number of spinal surgeries and increase the quality of life of AIS patients. For more information, please contact Jennifer Johansson at jen.johansson@liberatingtech.com.
Jennifer Johansson, MS, is senior research engineer at Liberating Technologies, Inc., a College Park Company.
References
1. Katz DE, et al. “Brace Wear Control of Curve Progression in Adolescent Idiopathic Scoliosis,” J Bone Joint Surg Am. 2010; 92:6:1343-1352.
2. Weinstein SL, et al. “Effects of Bracing in Adolescents With Idiopathic Scoliosis,” N Engl J Med. 2013; 369:16:1512-21.
The contents of this article were developed under a grant from the National Institute on Disability, Independent Living, and Rehabilitation Research (NIDILRR grant number 90BI0010). NIDILRR is a Center within the Administration for Community Living (ACL), U.S. Department of Health and Human Services (HHS). The contents of this article do not necessarily represent the policy of NIDILRR, ACL, or HHS, and you should not assume endorsement by the federal government.